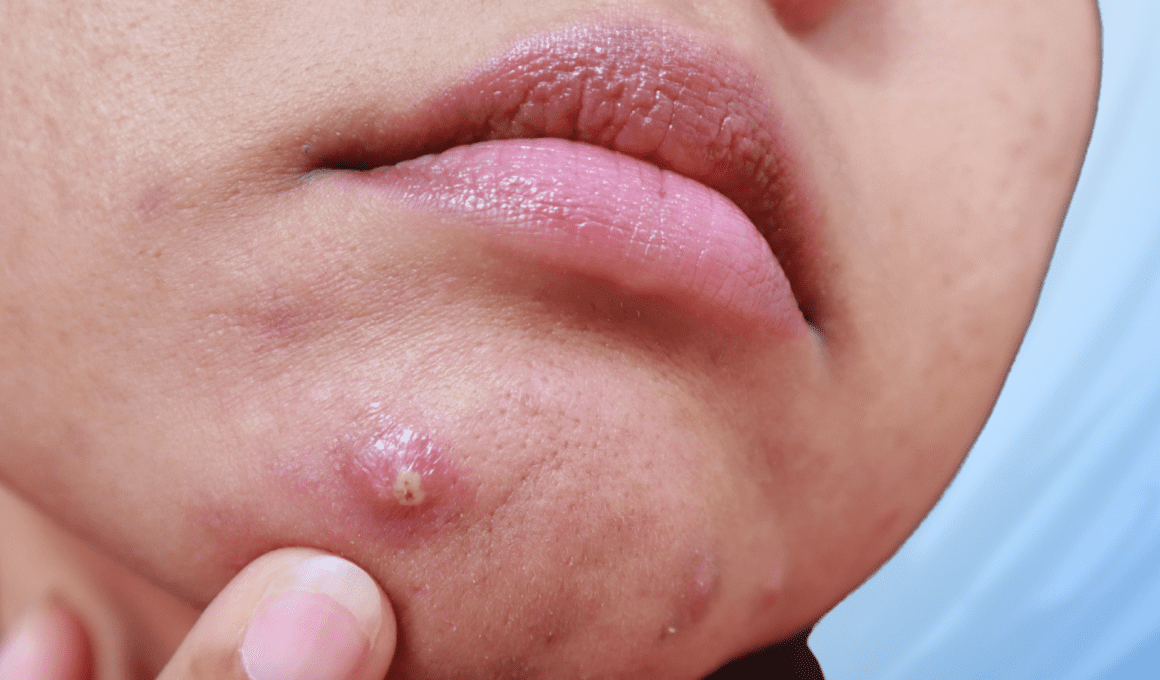
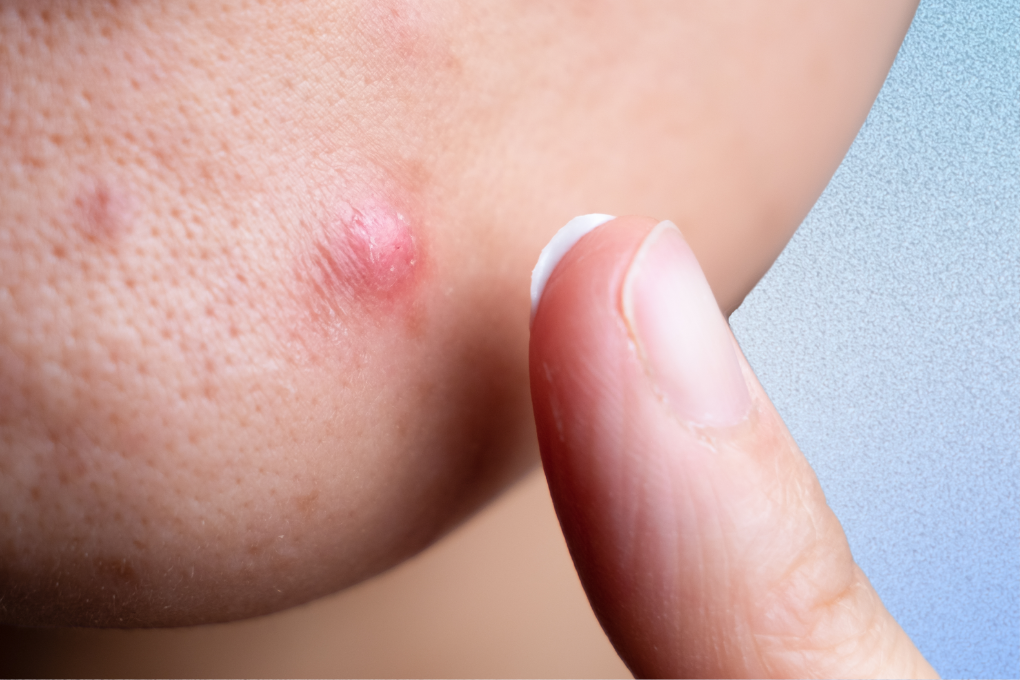
While most people experience mild to moderate acne at some point in their lives, some of us suffer from a more severe form of acne called cystic acne. Cysts are typically large and inflamed; they often don’t come to a head, and they can take weeks to heal. Sometimes, a cystic pimple is not visible as much as it is felt under the skin, and it can be very painful when you touch or press on it.
Cystic acne occurs when our pores become blocked with dead skin cells and excess oil. The resulting pimple gets trapped and ruptures under the skin, leading your body to form a pus-filled cyst to contain the perceived attack. Cystic acne usually appears on the face, neck, chest, and back, and can be extremely difficult to treat without professional help.
Cystic Acne Spot Treatment
Since cystic pimples can stay around for so long, we are all looking for ways to shrink them quickly. If you just have the rare cystic pimple, you’ll want to treat it immediately. However, because the cysts are so deep under the skin, they can be challenging to treat with spot treatments.
Pimple patches with microneedles that deliver medication, such as salicylic acid, into the skin can sometimes be effective on cysts, especially if they are used early, right when you first notice that deep and foreboding pain under your skin.
Hero Cosmetics Mighty Patch Micropoint for Early Stage Zits and Hidden Pimples with 0.5% Salicylic Acid and Niacinamide
The classic Mighty Patch from Hero Cosmetics has a Micropoint version to help target deep pimples. The hydrocolloid patch provides protection and a good environment for healing, while 395 dissolving micropoints deliver salicylic acid under the skin where it can be most effective. Niacinamide, hyaluronic acid, and centella extract help hydrate and soothe, so your skin can heal. Simply press the patch into your pimple for 20 seconds, then leave for 6-8 hours.
- Effective on deep pimples when used early
- Salicylic acid to unclog pores
- Hyaluronic acid, niacinamide, and centella extract to hydrate and soothe
- Expensive if you need them often
Benzoyl peroxide and sulfur spot treatments can also work to fight bacteria on the skin and to reduce the inflammation of a cyst. It’s good to have a spot treatment already on hand so you can use it at the first sign of an under-the-skin cyst taking root.
Dermalogica Deep Acne Liquid Patch Invisible Spot Treatment with 4% Niacinamide and 5% Sulfur
Dermalogica's Deep Acne Liquid Patch spot treatment was specifically designed for deep cystic pimples. It goes on as a liquid with 5% sulfur to help clear the breakout and dries into a semipermeable patch to protect the skin. Camphor provides a welcome cooling sensation that can help soothe the pain of a deep pimple, while niacinamide and lactic acid help to brighten and fade post-acne marks. As a bonus, it is safe for use during pregnancy.
- Camphor for pain from deep pimples
- Sulfur helps clear breakouts
- Niacinamide and lactic acid to help brighten acne marks
- Pregnancy safe
- Small amount
Kate Somerville EradiKate Acne Spot Treatment Clinically Formulated with 10% Sulfur, BHAs, and Zinc Oxide
Kate Somerville's EradiKate Acne Spot treatment is formulated with the maximum 10% sulfur to quickly treat pimples, salicylic acid to unclog pores, and zinc oxide to absorb excess oil. Use on surface pimples or as soon as you feel a deep one forming. Make sure the formula has settled and has not been shaken. Then insert a Q-tip through the clear alcohol layer into the pink sediment and apply this pink treatment directly to your pimple and let dry.
- Sulfur and salicylic acid to clear pimple
- Zinc oxide to control oil
- Alcohol may be strong for some skin types
While over-the-counter hydrocortisone cream can cause skin thinning and even pimples if used long term, it can be used as a spot treatment on cysts to help bring down inflammation and redness. If a cyst is forming and you have nothing else on hand, try icing it to bring down the inflammation and reduce the pain of deep cysts.
What Causes Cystic Acne?
While there are many things that contribute to cystic acne, it is a medical condition, and you did not do anything to cause it. If you still feel somehow to blame, remember that we all know people with clear skin who rarely wash their face, use any skin care or makeup products they want, and pay no attention to what they eat or drink. Some of us just have more acne-prone skin and need extra help.
Excessive oil production is one of the most common causes of cystic acne. When our skin produces too much oil, it can mix with dead skin cells and bacteria, clogging our pores and leading to deep acne breakouts.
There is often more than one factor that can combine to cause cystic acne, including:
Hormonal Changes
Is cystic acne hormonal? It can be. Hormonal fluctuations, especially during puberty, pregnancy, and menstruation, can cause our skin to produce more oil, which can clog our pores and lead to cystic acne. Hormonal acne can also be caused by polycystic ovary syndrome (PCOS), a hormonal disorder, which can cause your skin’s oil glands to produce more sebum, leading to clogged pores and acne.
Hormonal acne is increasingly common in adult women and often presents as cystic acne on the lower half of the face, the cheeks, jawline, chin, and neck.
Genetics
Acne can run in the family, so if your biological family members have had acne, you may be more likely to develop cystic acne.
Stress
Stress can trigger the release of hormones such as cortisol that can increase oil production and inflammation in the skin, potentially worsening acne.
Skincare and Makeup Products
Some products that we put on our faces contain ingredients that can cause or worsen acne. Any facial oils or oils in other products should be added carefully or avoided for those of us who break out easily. Other ingredients, such as bismuth oxychloride, an ingredient to provide shimmer in some makeup, can block our pores and cause acne. Pay attention to the ingredients in your skincare and makeup, and add new items slowly so you can determine if they are causing breakouts.
Diet
There is some evidence that suggests that insulin resistance may contribute to the development of acne. Foods with a high glycemic index can cause a rapid increase in blood sugar levels, which, in turn, triggers the release of insulin and other hormones, which may contribute to the development of acne. Additionally, refined carbohydrates might create an inflammatory response in the body, which can make acne worse.
Some people also have a sensitivity to dairy products that can cause or worsen acne. However, acne, especially more severe cystic acne, is a medical condition and cannot be treated with diet alone. If you have cystic acne, it is important to see a dermatologist before making dietary changes.
How to Treat Cystic Acne
While there are ways to treat and shrink cysts when they pop up, the best way to treat cystic acne is by going to your doctor. It is important to get medical treatment if you can because cystic acne is so deep that treatments on the surface of your skin often will not penetrate deep enough to help, and the risk of scarring is higher than with other types of acne.
Using Isotretinoin (Accutane)
Isotretinoin, also known as Accutane, is a powerful medication that reduces oil production in the skin and can prevent acne from forming. It belongs to a class of medications known as retinoids, which are derivatives of vitamin A. Accutane works by reducing the size and activity of the oil-producing glands in the skin. It also has anti-inflammatory properties, which can help reduce the redness and swelling associated with acne.
In general, Accutane is taken for 15-20 weeks, though treatment times can vary, and the recommended dosage is based on your weight. While Accutane is highly effective, it is associated with several potential side effects, so it is typically used under close medical supervision to treat severe acne that has not responded to other treatments.
Taking Hormonal Medication
When cystic acne in women is determined to be hormonal, using medication to correct the imbalance can be extremely effective in reducing acne. Birth control pills containing both estrogen and progestin can help regulate the hormonal fluctuations that contribute to acne.
Another option is spironolactone, a diuretic that is often used off-label to treat hormonal acne in women by reducing the effects of androgens on the skin, which can lead to a decrease in oil production and acne.
Taking Antibiotics
While isotretinoin and hormonal medications target oil production to reduce acne, antibiotic treatments target the bacteria involved in cystic acne.
Oral antibiotics, such as tetracycline or doxycycline, may be prescribed for cystic acne to reduce inflammation and kill bacteria in the short term. Antibiotics are often not prescribed long-term due to the risk of antibiotic resistance and the disruption they can cause in the balance of bacteria in our gut.
Prescription Topical Treatments
Cystic acne is difficult to treat with topical products since the lesions are so deep, but often prescription topicals are combined with oral medication to help keep pores clear.
Prescription-strength retinoids such as tretinoin (Retin-A), adapalene at 0.3 percent (Differin), and tazarotene (Tazorac) can increase skin cell turnover to help unclog pores and reduce inflammation. Topical antibiotics, prescription-strength azelaic acid, and combination treatments can also help to clear our pores.
Injections
Dermatologists can inject a corticosteroid into a cyst to reduce inflammation and speed up the healing process. This is more of a stopgap measure, and it is generally not used as a long-term solution for severe cystic acne.
At-Home Cystic Acne Treatment
Seeing a dermatologist is very important if you have cystic acne due to the risk of scarring. If you have cystic acne and are unable to see a doctor for medical treatment, you can use topical over-the-counter acne products to help reduce inflammation and treat any non-cystic pimples. Keep in mind that it is important to add acne treatments slowly and carefully to avoid damaging your skin barrier with too many harsh products.
Here are four common at-home cystic acne treatment options:
Benzoyl Peroxide
Benzoyl peroxide works by killing the bacteria that cause acne, reducing inflammation, and helping to unclog pores. When benzoyl peroxide is applied to the skin, it penetrates the hair follicles and pores, where it releases oxygen. This oxygen creates an environment that is toxic to the bacteria that cause acne.
You can find benzoyl peroxide in face washes and leave-on treatments in strengths ranging from 2.5-10 percent. If you have never used benzoyl peroxide before, try starting with a face wash in a lower strength to see how your skin reacts before trying a higher strength or a leave-on treatment. Also, be careful of your pillowcases and towels as benzoyl peroxide can bleach fabrics.
La Roche-Posay Effaclar Duo Dual Action Acne Cleanser with 4% Benzoyl Peroxide, LHA, and Niacinamide
Effaclar Duo Acne Cleanser is part of La Roche-Posay's acne-focused Effaclar line. It gets its name from its dual-action approach of treating breakouts and clearing pores to prevent new acne from forming. This face wash thoroughly cleanses the skin to remove excess oil while targeting acne-causing bacteria with 4% benzoyl peroxide and exfoliating with 0.1% lipo-hydroxy acid, a derivative of salicylic acid. It is also infused with La Roche-Posay's soothing prebiotic thermal water.
- Balanced strength
- Lipo-hydroxy acid to exfoliate
- Niacinamide and thermal water to soothe
- More expensive than other options
- Niacinamide can be irritating for some skin types
Naturium Cream Cleanser with 5% Micronized Benzoyl Peroxide and N-Acetyl Glucosamine
Naturium's cream cleanser has a moderate strength of 5% micronized benzoyl peroxide to clear and prevent breakouts without overpowering. It cleanses your skin without stripping it by ensuring an appropriate ph balance of 5.0-6.0 to help maintain your skin's hydration. The amino sugar N-acetyl glucosamine is added to the formula to help minimize dryness which is a common concern when using benzoyl peroxide.
- Moderate strength
- pH balanced
- N-aceytl glucosamine to minimize dryness
- May be too strong for sensitive skin
Paula's Choice CLEAR Extra Strength Clearing Treatment with 5% Benzoyl Peroxide
Paula's Choice Daily Skin Clearing Treatment with 5% benzoyl peroxide is designed as an extra-strength treatment for stubborn acne. It will help fight existing pimples and also work to prevent future breakouts while also soothing with allantoin and bisabolol. This lotion can be applied two times a day after cleansing and is lightweight enough to be used under makeup. For sensitive skin, try the 2.5% version first.
- Lightweight lotion with matte finish
- Leave-on benzoyl peroxide for stubborn acne
- Allantoin and bisabolol to soothe
- 5% benzoyl peroxide may be too strong for some skin types
Salicylic Acid
Salicylic acid is a type of beta-hydroxy acid (BHA) that works by penetrating into our pores and dissolving the sebum, dead skin cells, and other debris that can clog our hair follicles and lead to acne. It can help improve acne by reducing redness, inflammation, and excess oil on the skin’s surface.
Salicylic acid is available over-the-counter in face washes and leave-on treatments. Salicylic acid can be drying, and too much may make your skin irritated and peel, so start slowly by using products with salicylic acid only a few days a week at first before increasing, if needed.
Paula's Choice CLEAR Pore Normalizing Cleanser Acne Face Wash with 0.5% Salicylic Acid
This gentle salicylic acid cleanser from Paula's Choice helps dissolve pore-clogging oil and debris without irritating sensitive skin. A low strength of 0.5% salicylic acid in a gel texture will refresh your skin and clear your pores, while glycerin, arginine, and panthenol help soothe and hydrate. With this formula you can enjoy the benefits of salicylic acid without flaking or dryness.
- Lower strength 0.5% salicylic acid
- Good choice for sensitive skin
- Also comes in a refill pouch
- May not be strong enough for some skin types
La Roche-Posay Effaclar Medicated Gel Cleanser with 2% Salicylic Acid and LHA
La Roche-Posay's gel cleanser is our top choice for oily skin types because it thoroughly cleanses and dissolves oil with 2% salicylic acid. It was even tested to reduce excess surface oil by up to 47%, so it can help keep skin less oily during the day. It also contains lipo-hydroxy acid (LHA), which has exfoliating and skin renewing properties, and glycerin to help the skin retain moisture.
- Full strength 2% salicylic acid
- Added LHA to help exfoliate
- May be strong for sensitive skin
Paulas Choice Skin Perfecting BHA Liquid Exfoliant with 2% Salicylic Acid
Paula's Choice 2% BHA Liquid Exfoliant is a fan favorite for good reason. This lightweight toner refreshes skin and uses 2% strength of salicylic acid to exfoliate and clear pores. It has an optimal pH, which is important for exfoliants to get maximum effectiveness without irritation, and it contains soothing green tea to support the skin’s barrier. But watch out because this gentle formula is still strong, so remember to ease into use.
- Optimal pH for acid
- Green tea to soothe and support skin barrier
- Expensive
- Too strong for some skin types
Retinoids
Retinoids are a type of vitamin A derivative that are commonly used in skincare products to treat acne. They work by increasing cell turnover in the skin, which helps to prevent the buildup of dead skin cells and other debris that can clog pores. Retinoids also have anti-inflammatory properties and can help to regulate oil production in the skin.
You can find retinoids in the form of adapalene at 0.1 percent strength and retinol over-the-counter as leave-on treatments. Because retinoids work by increasing cell turnover, you may see a “purge” of more pimples being brought to the surface of your skin at first. Make sure to start slowly with your retinoid and expect to wait a few months before seeing an improvement.
La Roche-Posay Effaclar Adapalene Gel 0.1% Treatment
From La Roche-Posay's Effaclar line, which is designed for acne-prone skin, comes their adapalene 0.1% treatment gel. Adapalene is a prescription-strength retinoid available over the counter in the U.S. in 0.1% strength. It works by increasing cell turnover to help prevent acne and can be used to treat blackheads, whiteheads, clogged pores, pimples, and even KP bumps on the arms. La Roche-Posay's version comes in an effective fragrance-free gel that you apply in a thin layer to your face or body once a day.
- Maximum over-the-counter strength
- Non-greasy gel-like texture
- HSA and FSA eligible
- Expensive
The Ordinary Retinal 0.2% Emulsion High-Strength Stabilized Retinaldehyde Serum
The Ordinary has many different retinoid products to choose from, but their Retinal 0.2% Emulsion is their highest strength formula. While primarily advertised for aging, the retinaldehyde in this product is a one-step away from prescription tretinoin (the active form of vitamin A), making it a great retinoid entry point for acne-prone skin. This serum-textured formula will increase cell turnover, helping to remove dead cells that can clog pores.
- Retinaldehyde is a strong over-the-counter retinoid
- Airless pump to protect formula
- Light creamy serum texture
- Small amount
- Yellow hue can rub off on light fabrics
Sulfur
Sulfur has been historically used to help with skin conditions by going to natural hot springs that contain sulfur.
For acne, sulfur has mild exfoliating properties, which allow it to remove dead skin cells to stop them and other debris from blocking your pores, while also absorbing excess oil. Sulfur is antimicrobial, so it can help kill the bacteria that lead to acne. Sulfur is available over-the-counter in face washes, clay masks, and spot treatments. Although it can still irritate sensitive skin, sulfur is seen to be a gentler acne treatment than other options.
Kate Somerville EradiKate Daily Foaming Cleanser Acne Treatment with 3% Sulfur
Kate Somerville's EradiKate Daily Foaming Cleanser contains 3% sulfur to fight breakouts while still being gentle enough to use on a daily basis. This whipped sulfur foaming cleanser keeps pores clear and absorbs excess oil without overdrying. It is lightly fragranced to offset the sulfur smell. Massage onto skin for 30 seconds and even let it sit for 2-3 minutes on your T-zone as a mask before rinsing to help clear sebaceous filaments.
- 3% sulfur fights breakouts without overdrying
- Can also be used as a mask to clear sebaceous filaments
- Contains fragrance
- Expensive
Murad Rapid Relief Acne Clay Face Mask with Salicylic Acid and 5% Sulfur
The Rapid Acne Relief mask by Murad is made with 5% bacteria-fighting sulfur as well as exfoliating salicylic acid to tackle breakouts. Kaolin clay, which works to absorb excess oil and reduce shine, is balanced with hydrating Austrian peat extract to keep the mask from being too drying. The smell of sulfur is partially covered by eucalyptus oil, so you get the acne-fighting power with a spa night friendly scent.
- 5% sulfur fights breakouts
- Salicylic acid clears pores
- Kaolin clay absorbs excess oil
- Expensive for the size
What is the Difference Between Cystic Acne and Nodular Acne?
Cystic and nodular acne are both inflammatory acne, and their main difference is the type of lesion—cysts vs. nodules.
Both cysts and nodules are made when the clogged follicle ruptures under the skin and becomes inflamed from your body’s immune response to the spilled bacteria. If the inflammation then fills with pus, it becomes a cyst. Cystic acne is characterized by large, painful cysts filled with pus, while nodular acne consists of hard, painful bumps or nodules beneath the skin’s surface. Both cystic and nodular acne tend to be deep within the skin, with cystic acne often extending deeper. Similar to cystic acne, nodular acne can be difficult to treat and can lead to scarring.
Cystic Acne Scarring
The last step of dealing with cystic acne is addressing the scars it often leaves behind. The inflammation caused by cystic acne can damage the surrounding skin tissue, including the collagen and elastin fibers that give the skin its elasticity and firmness, resulting in the formation of scars.
Cystic acne scars can be either depressed (atrophic) or raised (hypertrophic). Atrophic scars are the most common type of cystic acne scars, leaving visible indentations in the skin, which are caused by the loss of tissue in the affected area. Atrophic scars can appear as shallow depressions or deep pits in the skin. They can also be classified as ice-pick scars, boxcar scars, or rolling scars, depending on their shape and depth. Hypertrophic or keloid scars, on the other hand, occur when the body produces too much collagen during the healing process, resulting in raised and thickened scars.
Unlike the red or brown marks of post-inflammatory hyperpigmentation, which can eventually fade with time and topical treatments, scars change the texture of the skin and do not usually go away without being treated by a dermatologist. Some of the techniques used to improve cystic acne scars include chemical peels, microneedling, laser therapy, dermal fillers, subcision, and dermabrasion.
Although it may be tempting to purchase at-home products that claim to reduce indented acne scars, it would be a better use of your money to save it and eventually consult a dermatologist for professional scar correction.
Cystic acne is painful to deal with, both physically and emotionally. When treating cystic acne, you should consult a dermatologist or medical professional as soon as possible to determine the best course of treatment for your case, as the effectiveness of each treatment can vary depending on the type and severity of your acne.
Be patient. Except for corticosteroid injections, nothing works overnight, and cystic acne can often be a long-term condition to manage. Although it sometimes seems like cysts wait to pop up just before a big event, don’t let cystic acne stop you from doing anything you want to do. Try to practice acne neutrality, cover pimples with makeup if needed, and continue to live your life while finding the right treatment and skincare routine for you.