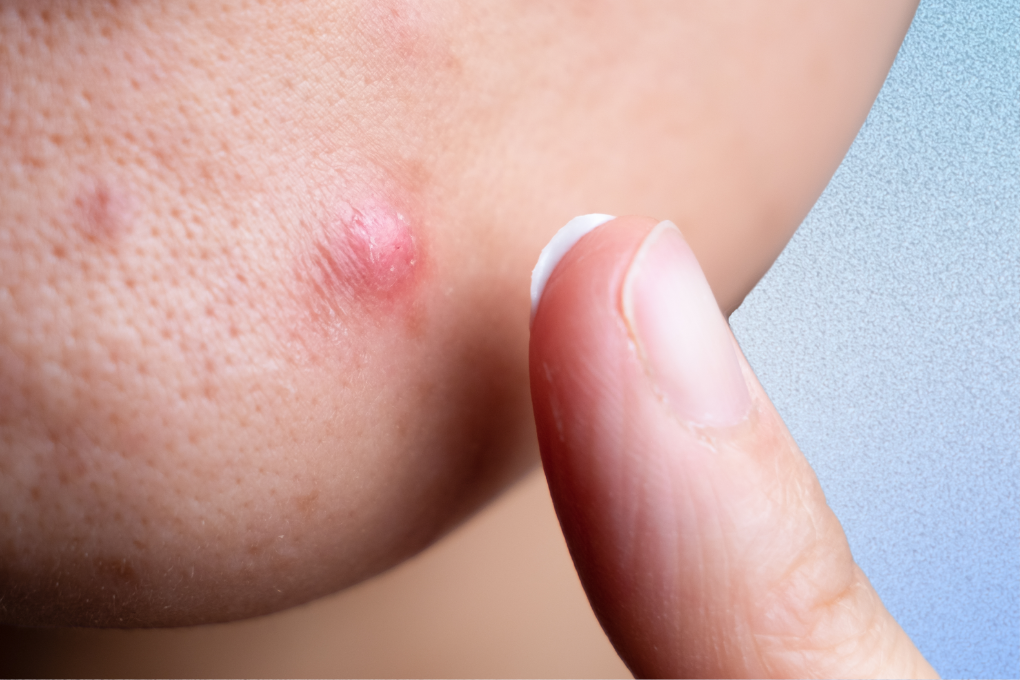
Struggling with persistent pimples that seem to defy acne logic? If you’ve ever experienced small, itchy red spots on your skin that didn’t improve with normal acne treatment, you may already be familiar with fungal acne.
What is Fungal Acne?
Known medically as Malassezia folliculitis or Pityrosporum folliculitis, fungal acne is not actually acne, even though the little red spots on the face might look similar to pimples.
Acne vulgaris, your run-of-the-mill bacterial acne, is caused by a combination of factors including excess sebum production, clogged hair follicles due to dead skin cells, and the presence of acne-causing bacteria (primarily Cutibacterium acnes). Fungal acne is not caused by bacteria or clogged pores, but by an overgrowth of yeast, specifically the Malassezia yeast which is naturally present on our skin.
This yeast, which is a type of fungus, thrives on sweat, oils, and other lipids, which can help it to grow out of control, leading to inflammation in the hair follicles. This inflammation can cause small, itchy red spots on the skin to form on your body and face that can mimic the look of traditional pimples.
What Causes Fungal Acne?
Malassezia yeast thrives in moist and oily environments. There are various triggers for the yeast overgrowth that causes fungal acne:
- Humid Climate: Living in or visiting humid areas can exacerbate fungal acne by encouraging yeast growth.
- Excessive Sweating: Especially when combined with heat and humidity, sweat can create a perfect environment for yeast to thrive.
- Compromised Immune System: A weakened immune system may struggle to regulate yeast, leading to these itchy red pimples on the face and body.
- Tight, Non-Breathable Clothing: Wearing tight clothes, especially while sweating, can trap moisture and facilitate fungal growth.
- Oral Antibiotics: Antibiotics can disrupt the natural skin flora, potentially leading to itchy red spots on the face due to an overgrowth of yeast.
- Oily Skin: As this yeast feeds on sebum, having naturally higher oil production may contribute to the yeast responsible for fungal acne.
- Occlusive Skincare Products: Heavy creams and oils can trap moisture, leading to an ideal environment for fungal acne to thrive.
- Hygiene: Infrequent washing or not showering after sweating can contribute to the growth of Malassezia yeast.
- Hormonal Changes: Fluctuations in hormones can change the skin’s environment, making it more susceptible to itchy red spots on the face and body.
- Oil-Based Products: Certain oils in skincare and hair products can exacerbate the condition, leading to these small, raised red bumps on the skin.
- Genetic Predisposition: Some individuals may be more genetically prone to fungal acne, experiencing itchy, raised bumps on the face more frequently.
While these factors can contribute to the development of fungal acne, they do not guarantee its occurrence. Your skin is unique, and what triggers fungal acne in one person may not affect another.
How to Identify Fungal Acne
Fungal acne’s little red spots on the face or body is often mistaken for traditional acne due to its appearance, but the causes and treatments differ significantly. Here’s how to differentiate between the two:
- Uniformity: Fungal acne is usually uniform in appearance—itchy red spots on the face or body or tiny bumps on the skin that are all roughly the same size and often appear in clusters. Unlike traditional acne, which can vary from the smaller closed comedones and blackheads to large cysts, the papules and pustules caused by fungal acne are usually uniform in size and appearance.
- Itching: Fungal acne is often irritated and itchy, which is a key symptom that differentiates it from bacterial acne. These itchy raised bumps on the face and body can cause significant discomfort and may worsen with heat, moisture, or when wearing tight clothing that doesn’t allow the skin to breathe. This can make activities like working out or being in a hot, humid environment particularly aggravating for the condition.
- Location: Fungal acne’s little itchy red spots on the skin love clustering together. Fungal acne tends to appear primarily in areas where there’s a lot of oil production or sweat, such as the forehead, chin, and chest.
Due to the similarities in appearance between fungal acne and bacterial acne, it can be challenging to diagnose the condition correctly without professional help. A dermatologist can provide an accurate diagnosis and treatment recommendations.
Fungal Acne vs. Closed Comedones
Both fungal acne and closed comedones are annoying, but knowing which one you’re dealing with can be half the battle. Fungal acne requires an antifungal approach, often involving topical antifungal creams or shampoos. In contrast, closed comedones benefit from treatments that unclog pores, such as salicylic acid or retinoids.
Having one does not preclude the other, so it is (unfortunately) possible to have both at the same time.
- Closed Comedones: These are genuine members of the acne family. Born from trapped sebum and dead skin cells inside the pore, they’re also commonly known as whiteheads. Because the top of the pore is closed, they look like tiny flesh-colored bumps, without the redness and inflammation of typical pimples. Unlike fungal acne, closed comedones are not typically itchy. They are caused by various factors, including an overproduction of oil, improper skincare, lack of exfoliation, and sometimes hormonal imbalances.
- Fungal Acne: Visually, fungal acne manifests as small, itchy red spots on your skin that tend to cluster up. It is usually found in areas where there’s a lot of oil production or sweat, such as the forehead, chest, and back. Fungal acne’s itchy nature sets it apart from closed comedones, and the pattern of breakout (clustered rather than scattered) is another distinguishing factor between the two. Traditional treatments that work for closed comedones might not do anything to improve fungal acne.
Fungal Acne Treatment
One of the challenges with fungal acne is that traditional acne treatments might not address the root cause. Instead of retinoids or salicylic acid, treating fungal acne involves antifungal medications and lifestyle changes to minimize the yeast growth on the skin.
As a first line of treatment, topical creams and medicated shampoos that contain active antifungal ingredients like ketoconazole or pyrithione zinc can reduce the yeast population on the skin. Maintaining a routine that reduces sweating and oil buildup can also help manage the condition. In more persistent or severe cases, oral antifungals such as fluconazole prescribed by a doctor may be necessary.
Fungal Acne Treatment at Home
Treating fungal acne at home requires a different approach than dealing with bacterial acne. Certain over-the-counter treatments and lifestyle adjustments can help maintain balance on the skin and support the management of mild fungal acne:
- Antifungal Ingredients: Look for over-the-counter products containing antifungal active ingredients such as ketoconazole or clotrimazole cream. Shampoos with ketoconazole, originally intended for dandruff (which is also caused by Malassezia yeast), can be applied to the affected skin during a shower, left on for a few minutes, and then rinsed off. Anti-dandruff shampoos containing zinc pyrithione or selenium sulfide and soaps with antifungal ingredients can also be effective.
- Topical Sulfur: Sulfur is antifungal, and sulfur-based treatments can help by suppressing the yeast and reducing inflammation. These are often available over the counter in ointments, soaps, and masks.
- Skincare Routine: Opt for fungal acne-safe cleansers, moisturizers, and other skincare products to reduce the chance of further feeding the yeast. Products labeled as “non-comedogenic” or “oil-free” are a good place to start when looking for suitable options. Check that your hair care products are also free of ingredients that trigger fungal acne or make sure that they don’t come in contact with your skin. Be consistent about showering and wash off any sweat so it doesn’t linger on your skin.
- Dietary Adjustments: There’s some evidence that yeast may flourish on sugars and refined carbohydrates. Reducing the intake of such foods could potentially help in controlling fungal acne.
- Loose Clothing: Tight clothing can trap heat and moisture, which creates an ideal environment for yeast to grow. Change out of wet or sweaty clothes quickly and opt for loose, breathable fabrics, such as natural fibers, or moisture-wicking materials to keep the skin dry and cool. If you need to wear a face mask, change it often as it can create a moist environment for yeast to thrive.
If you are experiencing persistent itchy red dots on the skin, or if you’ve tried over-the-counter remedies and have not seen improvement, it is time to consult with a dermatologist. A professional can confirm whether you have fungal acne or another skin condition and can prescribe the appropriate treatment.
Fungal Acne Ingredient Checker
Fungal acne ingredient checkers are tools designed to help you identify whether skincare or cosmetic products contain ingredients that could exacerbate or contribute to fungal acne. Since fungal acne is caused by an overgrowth of yeast that feeds on certain types of oils and lipids, these checkers analyze the ingredients in products to ensure they don’t contain anything that would be potentially problematic.
Using fungal acne-safe products can help deprive the yeast of its food source. Here are a few online fungal acne ingredient checkers that flag ingredients that can impact fungal acne:
To use these ingredient checkers, you typically input the full list of ingredients from a skincare product into the checker. The tool then cross-references these ingredients with a database and will flag anything known to promote the growth of fungal acne-causing yeast.
There you have it—the lowdown on fungal acne. Along with other skin conditions like rosacea and perioral dermatitis, fungal acne is an excellent mimic of standard bacterial acne and it’s a lesson that things are not always what they seem. Understanding fungal acne is the first step, and with an adjusted skincare routine and lifestyle habits, you are well on your way to keeping this yeast in check.