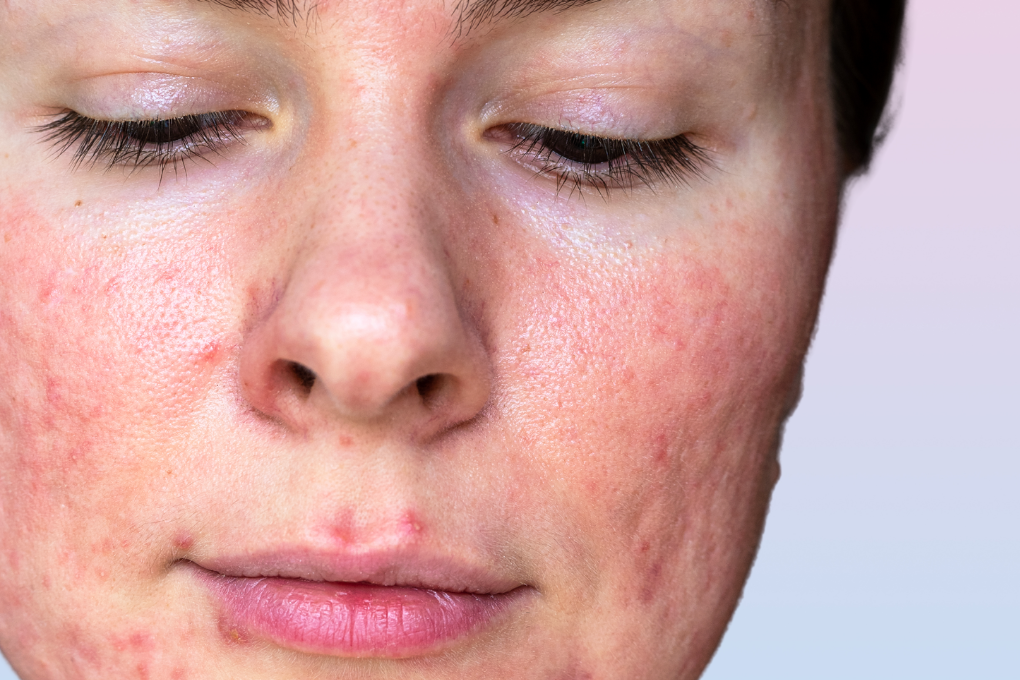
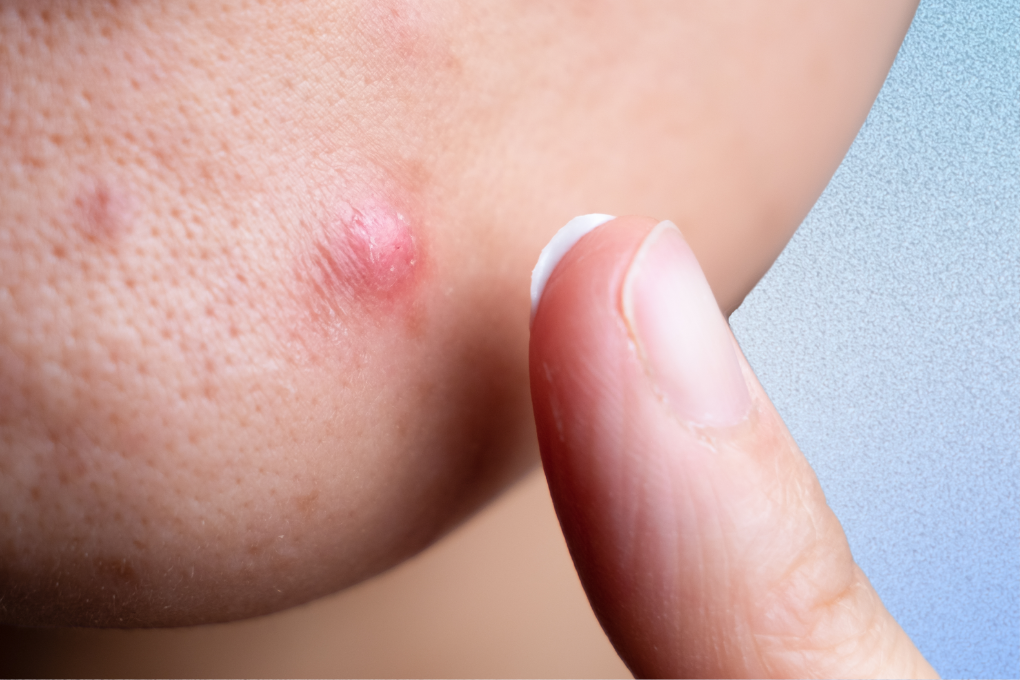
When you’re struggling with red and pus-filled bumps on your face, your first thought is probably to treat them like acne. However, rosacea pustules are also small, red, and filled with pus, much like traditional pimples.
If your pimples aren’t responding to normal acne treatment and are accompanied by a general redness and sensitivity, your acne may actually be rosacea pustules.
What Are Rosacea Pustules?
Rosacea is a skin condition that often shows up as redness on your face. Pustules from rosacea are small, pus-filled bumps that can appear on the skin during a papulopustular rosacea flare-up. Rosacea pustules are formed when inflammation is triggered in the skin and leads to the development of these pustules.
Rosacea pustules are different from acne in that they are primarily driven by inflammation and typically lack comedones (blackheads and whiteheads) that are characteristic of acne. Managing these pustules often involves anti-inflammatory treatments and addressing the underlying triggers.
Unlike acne, rosacea pustules are typically accompanied by other symptoms such as facial redness, visible blood vessels, and they may be triggered by factors including stress, diet, and changes in the weather. While it can be tempting to pop rosacea bumps, try to avoid doing so because popping them can exacerbate inflammation, potentially leading to more severe irritation or scarring.
What Is Papulopustular Rosacea?
Papulopustular rosacea is a subtype of rosacea that often gets mistaken for acne due to its similar appearance. It is sometimes called inflammatory rosacea or acne rosacea. While classic rosacea primarily involves facial redness and visible blood vessels, papulopustular rosacea also includes red bumps (papules) and pus-filled bumps (pustules), resembling acne.
Papulopustular rosacea can include common symptoms of rosacea, such as skin sensitivity and flushing.
The exact cause of all types of rosacea, including papulopustular, isn’t fully understood. However, it is believed to involve a combination of genetic, environmental, and immune system factors. Potential triggers for rosacea—such as sun exposure, emotional stress, hot or cold weather, wind, alcohol, spicy foods, certain skincare products, microscopic mites, and bacteria—can exacerbate this skin condition. Additionally, there’s some discussion about a link between rosacea and the gut, but more research is needed to understand these connections fully.
How to Get Rid of Rosacea Pustules?
Differentiating between rosacea and other skin conditions, such as acne, is the first step to getting rid of pustules from rosacea, and consulting a dermatologist will ensure you get an accurate diagnosis and the most effective treatment plan. Since the cause of rosacea is not fully understood, ongoing management and treatment are often necessary.
Work closely with your doctor on your rosacea so they can help monitor the effectiveness of the treatment and make adjustments as needed.
Treating rosacea pustules involves a combination of lifestyle changes, over-the-counter products, and medical treatment such as:
Gentle Skincare for Rosacea
Rosacea skin can be super sensitive. Keep a simple skincare routine and opt for gentle face cleansers and moisturizers, and avoid anything too harsh or abrasive. Some brands have sensitive skin or “anti-redness” lines that are better for rosacea.
Paula's Choice CALM Nourishing Milky Toner for Sensitive Skin and Redness
Paula's Choice Nourishing Milky Toner from their Calm line of products is full of skin-replenishing ingredients and antioxidants to soothe redness and sensitivity by supporting the skin barrier. Hyaluronic acid and glycerin hydrate the skin, while allantoin, panthenol, and marshmallow root extract help reduce redness and calm the skin. This toner is designed to strengthen the skin barrier to prevent future sensitivity, making it an excellent choice if your skin is irritated from harsh acne treatments.
- Gentle for sensitive and rosacea-prone skin
- Strengthens skin damaged from acne treatments
- Supports skin barrier to prevent future sensitivity
- Expensive for the size
EltaMD Skin Recovery Lightweight Moisturizer for Damaged Skin Barrier with Amino Acids
Elta MD's Skin Recovery Light Moisturizer is a weightless lotion designed with acne-prone and sensitive skin in mind. It uses the brand's patented AAComplex of amino acids to restore the skin's natural barrier, which makes it one of our favorite moisturizers to use alongside a strong acne treatment. With hyaluronic acid, glycerin, squalane, and coconut extract, this lotion soothes and moisturizes dehydrated skin while calming irritation and redness.
- Lightweight with hydrating ingredients
- AAComplex restores skin barrier
- Great option when using harsh acne treatments
- Expensive
Azelaic Acid for Rosacea
Azelaic acid is effective in managing rosacea due to its potent anti-inflammatory properties. By calming the skin’s inflammatory response, azelaic acid helps alleviate redness and soothe the associated discomfort. Certain microorganisms are also present in rosacea, and azelaic acid is able to inhibit their growth thanks to its antimicrobial properties. Additionally, azelaic acid can help with regulating cell turnover to decrease the acne-like bumps.
You can get serums and creams with azelaic acid over the counter, while higher strengths are available by prescription.
Paula's Choice 10% Azelaic Acid Booster with Licorice and 0.5% Salicylic Acid
This 10% Azelaic Acid Booster from popular skincare brand Paula's Choice is one of the strongest azelaic acid products available over the counter. The azelaic acid is combined with 0.5% salicylic acid to fight acne, fade hyperpigmentation, and reduce redness. It comes in a lightweight gel-cream formula that can be applied by itself or mixed with a serum or moisturizer to simplify your routine.
- Great for sensitive or rosacea-prone skin
- Reduces redness, fights acne, and fades marks
- Can be mixed with other skincare products
- Expensive for the amount
Proactiv Clean Azelaic Pore Perfector Cream Serum with 5% Azelaic Acid
Proactiv's Azelaic Pore Perfector Serum is a great choice for sensitive skin with mild acne or occasional breakouts. It's a lightweight lotion-like serum that's made with 5% azelaic acid, which can help decongest pores and reduce redness and hyperpigmentation. The hydrating formula includes squalane, bisabolol, and allantonin to soothe and moisturize.
- Lotion-like serum texture
- Squalane, bisabolol, and allantonin soothe and moisturize
- 5% azelaic acid gently clears pores
- May not be strong enough for some people
THAYERS Let's Be Clear Water Cream with 3% Azelaic Acid
Thayer's Let's Be Clear Water Cream is a gel moisturizer designed to help balance oily and combination skin while reducing redness. Along with hyaluronic acid to hydrate, this formula contains licorice root, which can help soothe and brighten skin. This moisturizer's star ingredient is azelaic acid, which can help clear skin while reducing redness and post-inflammatory hyperpigmentation. The 3% strength will be gentle enough for sensitive skin.
- Lightweight gel moisturizer
- Licorice root soothes and brightens
- 3% azelaic acid to gently clear and reduce redness
- Strength may be too low for some people
Sun Protection for Rosacea
Protecting your face from the sun with a broad-spectrum sunscreen with at least SPF 30 is crucial, even on cloudy days. If your skin is sensitive to sunscreen, look at gentle formulations with physical filters like zinc oxide. Tinted sunscreens can be helpful in toning down the redness.
La Roche Posay Anthelios Sunscreen UV Clear with Azelaic Acid Broad Spectrum SPF 50
Anthelios UV Clear Sunscreen from La Roche Posay was specifically designed for acne-prone and rosacea-prone skin. Its barely-there lightweight texture is noncomedogenic, and it uses azelaic acid to brighten and gently fight acne. Cell-Ox Shield Technology combines UVA and UVB protection with antioxidant protection to defend skin from free radicals caused by the sun. It soothes and hydrates and dries down to a natural finish.
- Barely-there texture with invisible finish
- Azelaic acid to brighten and fight acne
- Not water-resistant
Colorescience Sunforgettable Total Protection Face Shield Flex Tinted Mineral Sunscreen SPF 50
Colorescience is known for mineral SPF products, and Face Shield Flex is our favorite of their tinted sunscreens. What makes it stand out is the encapsulation of iron oxide pigments in the formula. So even though the sunscreen comes out white, it will "bloom" to the right color as you apply it to your skin, giving you an adaptable and buildable coverage. The six shades cover a range of skin tones, making it easier to find a match that will blend in with your skin. Colorescience's patented EnviroScreen® Technology protects from UVA and UVB rays as well as blue light, pollution, and infrared radiation.
- Six shades with adaptable medium coverage
- Water-resistant for 40 minutes
- Protects from blue light, pollution, and infrared radiation
- Niacinamide can be irritating for some people
Avoid Triggers
This can vary from person to person, so keeping a diary of what you eat, drink, and do can help identify what sets off your rosacea. Avoid triggers that can cause your flare-ups, such as sun exposure, extreme temperatures, stress, alcohol consumption, spicy foods, and certain skin or hair products.
Professional Help
A dermatologist can offer prescription treatments like topical creams or oral medications to target rosacea pustules. These medications can help manage symptoms and reduce the number of flares. Laser treatment can also be used to remove visible blood vessels and redness. A dermatologist can recommend the most suitable laser option based on your skin type and individual case of rosacea.
Rosacea vs. Acne
Rosacea pustules may look like acne, but they’re different skin conditions and each needs its own special approach. Keep in mind that they are not mutually exclusive; it is possible to have both acne and rosacea at the same time. Because their treatments will differ, it’s important to differentiate between acne and rosacea by consulting a dermatologist for proper diagnosis if you are unsure.
Understanding what’s acne and what’s rosacea will help you to give your skin the care it deserves. Here are some key differences of rosacea vs. acne:
Age of Onset
Acne most commonly begins during puberty, a time when hormonal changes lead to increased oil production and the potential clogging of skin pores. This makes acne a common struggle among teenagers, but for many people, particularly women, it can continue into or start in adulthood.
Rosacea, on the other hand, is rare in adolescents and typically emerges after the age of thirty. Sometimes adults unexpectedly dealing with rosacea will confuse it with late-onset adult acne.
Location
Acne can manifest on various parts of the body, but is most frequently seen on the face, chest, and back. These areas are prone to higher oil production, contributing to the development of pimples. Rosacea primarily targets the central portion of the face, including the cheeks, nose, forehead, and chin. This concentration on the face, particularly in areas prone to flushing, is the distinctive feature of rosacea.
Types of Blemish
Papulopustular rosacea shows up as red patches, swollen red bumps and pus-filled pustules on the face that may resemble acne, and visible tiny blood vessels. Some people with rosacea may also experience skin thickening, especially around the nose. However, unlike acne, papulopustular rosacea typically lacks open and closed comedones and deeper cysts or nodules that come from clogged pores and bacteria.
Skin Texture
The texture of your skin can provide clues to differentiate between acne and rosacea. Acne-prone skin often appears oily and may have a greasy surface, contributing to the blockage of pores. Rosacea-affected skin is typically dry and sensitive, with a tendency to react to skin products or environmental factors, leading to irritation and redness.
Facial Redness
Rosacea skin may feel tender and appear flushed, which is less common in acne. This condition is often accompanied by other symptoms of rosacea such as facial redness and visible blood vessels. In darker skin tones, the redness of rosacea can be less visible, but the papules and pustules will be noticeable. Rosacea often includes a burning or stinging sensation, especially when topical products are applied or certain triggers affect the skin.
Triggers
The triggers for acne and rosacea vary significantly. Acne is often influenced by oil production and hormonal changes, especially during puberty, pregnancy, or certain menstrual phases. Rosacea’s flare-ups can be prompted by a range of external factors, including certain foods (like spicy dishes), temperature changes, stress, and alcohol consumption.
Understanding and avoiding personal triggers is a critical part of managing rosacea.
Remember, whether it’s rosacea pustules or acne that is causing the breakouts on your face, understanding your skin is key. Differentiating between rosacea and acne, finding the right skincare routine, and seeking professional help will help you give your skin what it needs to be healthy and happy.