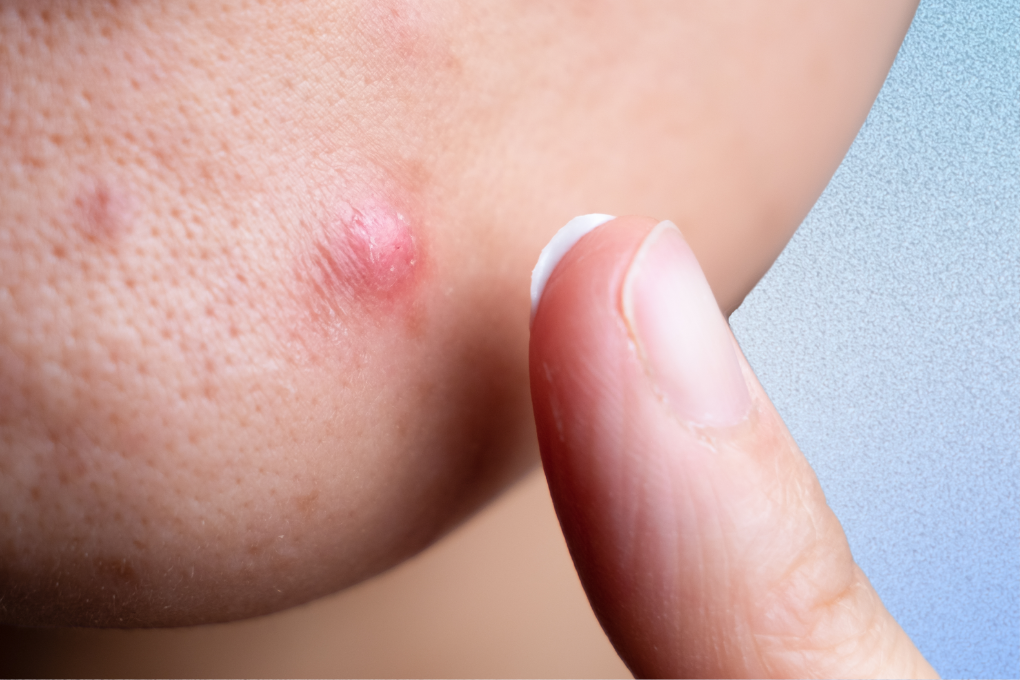
How is it that some people wash their face with shampoo as their only skin care step and have clear skin, while many of us have meticulous acne-fighting skincare routines and still get blemishes? Given that you are reading Acne Club, there’s a good chance that you are also in the acne-prone skin group.
What is Acne-Prone Skin?
Acne-prone skin tends to develop acne more often than other skin types. While most people experience pimples while going through puberty, some will experience worse breakouts or deal with it longer well into adulthood. They might label their skin as acne-prone to help find the right products for their skin. This skin type tends to have excess oil production and may be quite sensitive, leading to frequent breakouts.
Understanding the acne-prone skin type is important to be able to effectively manage and treat it. Common characteristics of acne-prone skin are:
- Oily Surface: Excess sebum gives the skin a greasy appearance.
- Frequent Breakouts: Regular occurrence of various types of acne.
- Sensitive Reaction: Prone to irritation and inflammation.
What Causes Acne-Prone Skin?
Acne-prone skin is a broad term that describes skin that frequently has blackheads, whiteheads, pimples, and sometimes more severe forms like cysts and nodules. There are several different ways this acne can be caused, including:
Extra Sebum
Sebum is an oily substance produced by your sebaceous glands to moisturize your skin. It plays a vital role in maintaining the skin’s moisture and protecting it from external contaminants. However, when your skin produces too much sebum, it can mix with dead skin cells and block hair follicles.
Excess sebum also creates an ideal environment for the acne-causing bacteria Cutibacterium acnes (C. acnes) to thrive, which can cause inflammation in your blocked pores leading to red angry pimples.
Microbiome
Your skin has its own set of bacteria, fungi, and viruses, known as the microbiome, which can influence acne. The bacteria C. acnes is commonly present on human skin and can help protect our skin, but they can also contribute to acne for some of us. Research has indicated that there’s a diverse population of C. acnes strains, some of which are more likely to contribute to acne development than others. The type that is naturally prevalent on your skin can contribute to it being acne-prone or acne-free.
Additionally, the yeast Malassezia, which lives on your skin, can sometimes overgrow and cause red bumps on your face that look like acne, but is actually Malassezia folliculitis or fungal acne.
Cell Turnover
Normally, skin cells turn over and shed regularly, but in acne-prone skin, this process might not be as effective.
If dead skin cells don’t shed properly, they can mix with excess sebum (oil) and clog pores. This clogging is a primary factor in the development of acne because it creates an environment for acne-causing bacteria to grow and cause inflammatory acne. If you naturally have a slower or irregular cell turnover, this can increase the likelihood that you’ll regularly experience clogged pores and breakouts.
Hormones
Fluctuations in hormones, such as androgens, can trigger sebaceous glands to make more sebum and cause your skin to be oily, leading from blackheads and whiteheads to cystic acne. Hormonal acne often appears on the jawline, chin, and lower face.
In addition to the standard above treatments for oily acne-prone skin, if you are female, your dermatologist may also suggest a medication to target these hormones. Birth control pills and anti-androgens like spironolactone and the topical treatment Winlevi can be effective in addressing the androgens that trigger excess sebum production.
Acne-Prone Skin Routine
For those of us with acne-prone skin, most of the battle is finding a skincare routine that balances effective acne treatments with keeping our skin healthy and hydrated. Too many harsh active ingredients can irritate our skin and damage our skin barrier. And too many nourishing ingredients without treating acne can often cause clogged pores and pimples.
Look for products designed for acne-prone skin that won’t clog your pores and adapt each step to your skin’s specific needs and responses. A dermatologist can offer the most tailored advice for your situation. A standard routine for acne-prone skin that strikes a balance between managing acne and maintaining overall skin health would look something like this:
Cleanser
Begin with a gentle cleanser to remove excess oil and impurities without stripping the skin.
Bioderma Sensibio Soothing Micellar Cleansing and Makeup Removing Foaming Gel for Sensitive Skin
This cleansing gel from French brand Bioderma's Sensibio line for sensitive skin uses micellar technology to gently cleanse and remove makeup. These cleansing microdroplets, or micelles, can capture oil and impurities without stripping, making this cleanser an excellent option for anyone with sensitive skin. It also uses Bioderma's patented D.A.F. complex, which works on all skin types to help improve the skin's tolerance threshold.
- Micelles gently cleanse and remove makeup
- Non-stripping for sensitive skin
- D.A.F. complex to increase skin tolerance
- More expensive than other options
Treatment
Applying targeted acne treatments with ingredients like salicylic acid, benzoyl peroxide, topical retinoids, and azelaic acid can help clear pores and calm inflammatory acne.
La Roche-Posay Effaclar Adapalene Gel 0.1% Treatment
From La Roche-Posay's Effaclar line, which is designed for acne-prone skin, comes their adapalene 0.1% treatment gel. Adapalene is a prescription-strength retinoid available over the counter in the U.S. in 0.1% strength. It works by increasing cell turnover to help prevent acne and can be used to treat blackheads, whiteheads, clogged pores, pimples, and even KP bumps on the arms. La Roche-Posay's version comes in an effective fragrance-free gel that you apply in a thin layer to your face or body once a day.
- Maximum over-the-counter strength
- Non-greasy gel-like texture
- HSA and FSA eligible
- Expensive
Paulas Choice Skin Perfecting BHA Liquid Exfoliant with 2% Salicylic Acid
Paula's Choice 2% BHA Liquid Exfoliant is a fan favorite for good reason. This lightweight toner refreshes skin and uses 2% strength of salicylic acid to exfoliate and clear pores. It has an optimal pH, which is important for exfoliants to get maximum effectiveness without irritation, and it contains soothing green tea to support the skin’s barrier. But watch out because this gentle formula is still strong, so remember to ease into use.
- Optimal pH for acid
- Green tea to soothe and support skin barrier
- Expensive
- Too strong for some skin types
Paula's Choice CLEAR Regular Strength Daily Skin Clearing Treatment with 2.5% Benzoyl Peroxide
Paula's Choice Daily Skin Regular Strength Clearing Treatment comes in a balanced 2.5% benzoyl peroxide in a leave-on treatment. With soothing allantoin and bisabolol, it will work to calm existing pimples while fighting acne-causing bacteria to prevent future breakouts. For more stubborn acne that does not respond to the regular strength, you can try the extra-strength version with 5% benzoyl peroxide.
- Lightweight lotion with matte finish
- 2.5% benzoyl peroxide is gentle yet effective
- Allantoin and bisabolol to soothe
- May not be strong enough for stubborn acne
Paula's Choice 10% Azelaic Acid Booster with Licorice and 0.5% Salicylic Acid
This 10% Azelaic Acid Booster from popular skincare brand Paula's Choice is one of the strongest azelaic acid products available over the counter. The azelaic acid is combined with 0.5% salicylic acid to fight acne, fade hyperpigmentation, and reduce redness. It comes in a lightweight gel-cream formula that can be applied by itself or mixed with a serum or moisturizer to simplify your routine.
- Great for sensitive or rosacea-prone skin
- Reduces redness, fights acne, and fades marks
- Can be mixed with other skincare products
- Expensive for the amount
Lightweight Hydration
Adding extra layers of lightweight hydration, also called skin flooding, is a great way to add extra moisture to acne-prone skin without relying on heavy products that might clog pores.
Moisturizer
It’s a common misconception that acne-prone skin doesn’t need moisturizing. Opt for a lightweight moisturizer or gel moisturizer to hydrate without causing further breakouts.
La Roche-Posay Toleriane Sensitive Fluide Lightweight Protective Moisturizer with Niacinamide
The Toleriane Sensitive Fluide is an oil-free moisturizer from La Roche-Posay's sensitive skin line. What makes it unique is its limited number of ingredients, which can help you avoid irritation if you have sensitive skin. Made with La Roche-Posay thermal spring water, niacinamide, and glycerin, it can hydrate your skin for up to 48 hours and also helps to support your moisture barrier. It is lightweight and moisturizing with a mattifying texture, making it a great option if you have skin that is both sensitive and acne-prone.
- Lightweight with mattifying texture
- Thermal water, niacinamide, and glycerin to hydrate and soothe
- Expensive
- Niacinamide can be irritating for some skin types
Sun Protection
Daily sunscreen application protects the skin from UV damage and can prevent post-inflammatory hyperpigmentation left behind after pimples from worsening.
Colorescience Sunforgettable Total Protection Face Shield Flex Tinted Mineral Sunscreen SPF 50
Colorescience is known for mineral SPF products, and Face Shield Flex is our favorite of their tinted sunscreens. What makes it stand out is the encapsulation of iron oxide pigments in the formula. So even though the sunscreen comes out white, it will "bloom" to the right color as you apply it to your skin, giving you an adaptable and buildable coverage. The six shades cover a range of skin tones, making it easier to find a match that will blend in with your skin. Colorescience's patented EnviroScreen® Technology protects from UVA and UVB rays as well as blue light, pollution, and infrared radiation.
- Six shades with adaptable medium coverage
- Water-resistant for 40 minutes
- Protects from blue light, pollution, and infrared radiation
- Niacinamide can be irritating for some people
La Roche-Posay Anthelios Light Fluid Face Sunscreen Broad Spectrum SPF 60
The Anthelios Light Fluid Sunscreen from La Roche-Posay is a fan favorite for a fast-absorbing, very lightweight sunscreen with a matte finish. If you usually hate the feeling of sunscreen on your face, this might be a good one for you to try. This chemical sunscreen is formulated for sensitive skin and also includes antioxidant protection to prevent sun damage. It contains alcohol to help it absorb quickly and is water-resistant for 80 minutes, making it a particularly good option for sweaty summer weather.
- Lightweight and fast-absorbing
- Water-resistant for 80 minutes
- Antioxidant protection
- Alcohol may be irritating for some skin types
Remember that having acne-prone skin does not mean you will always have acne, and having acne does not mean you are doing anything wrong compared to people with effortlessly clear skin. It also means that the skin care products those people use and love might not be the right choice for you. Use this self-knowledge as a tool to find the right products and treatments that work for you and your skin.